Commissioner’s message
As the next wave of COVID-19 sweeps across the country and enters increasing numbers of aged care settings, it is imperative for aged care providers to remain alert and take all reasonable precautions to protect the health and wellbeing of their consumers and workforce.
The ‘Winter Plan – A guide for residential aged care providers’ developed by the Department of Health and Aged Care and recently released by Minister Anika Wells, aims to help providers with their readiness, response and recovery from exposures and outbreaks of COVID-19 and/or influenza during winter this year.
While this plan is largely focussed on aged care in residential settings given the increased risk of transmission in a co-located living environment, it also includes an in-home care checklist.
As emphasised in the Winter Plan, up-to-date vaccination for both aged care residents and staff provides the best protection against COVID-19. However, it is not a perfect shield against infection which, for some people, may lead to severe illness and hospitalisation. For this reason, antiviral therapies should be an early consideration for adults in high-risk groups – including aged care residents – who test positive to the virus, irrespective of their vaccination status.
Oral antiviral treatments for COVID-19 are a key additional strategy to help keep people out of hospital and stop COVID-19 illness from becoming severe. The COVID-19 oral antiviral treatments, nirmatrelvir and ritonavir (Paxlovid®) and molnupiravir (Lagevrio®), are both available on the Pharmaceutical Benefits Scheme (PBS) and can be accessed through community pharmacies.
In line with the latest evidence, people aged 70 years or older can be prescribed COVID-19 antiviral treatments when they test positive, regardless of risk factors or the presence of symptoms. People aged 50 years or older can access these therapies where 2 risk factors are present, including living in residential aged care, chronic respiratory symptoms, kidney failure or diabetes. Medical assessment of an individual is a prerequisite for any prescription of an antiviral medication.
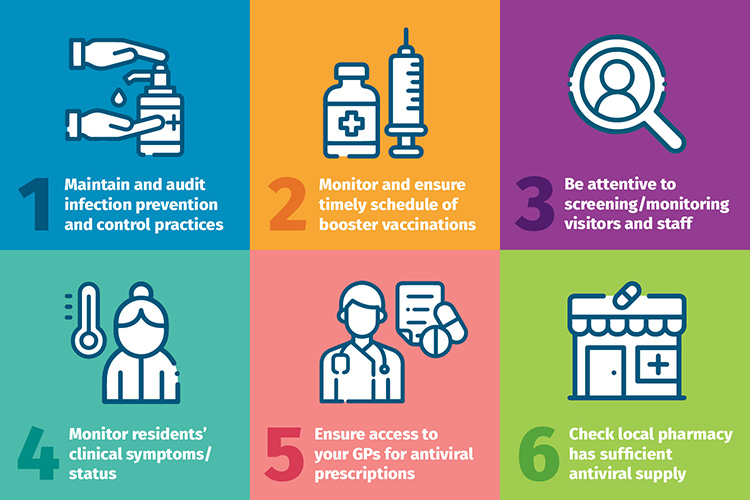
I recently emailed a letter to all residential aged care providers about ensuring you consider antiviral therapies as an early treatment for aged care residents who test positive to the virus. Alongside that correspondence, the Commission’s Chief Clinical Advisor Dr Melanie Wroth sent a clinical alert to all providers about being on guard against this current wave and the steps below that you must take to minimise the risks to older people for whom you provide care.
There is now overwhelming evidence that a slow or ineffective response to an outbreak places both residents and staff at increased risk of harm. In this circumstance, the Commission must consider whether to take regulatory action. Clearly, it is far better for providers to avoid this situation by being well-prepared for immediate and effective activation of your outbreak management plan so as to minimise any impact on the safety, health and wellbeing of residents in your care.
Serious Incident Response Scheme – important resource updates
We have updated a few of our Serious Incident Response Scheme (SIRS) resources for residential aged care providers to clarify reportable incidents involving unlawful sexual contact or inappropriate sexual conduct.
We consider any incidents involving unlawful sexual contact or inappropriate sexual conduct to be Priority 1 reportable incidents. This means that you must report these to us via the My Aged Care portal within 24 hours of becoming aware of the incident.
You must also report incidents that are unlawful or considered to be of a criminal nature (for example, sexual assault) to police within 24 hours. If you’re unsure whether an incident is a crime, report it to the police. Police are the appropriate authorities to investigate and identify whether an incident may involve criminal conduct.
We have now updated our ‘Serious Incident Response Scheme – Guidelines for residential aged care providers’ resource to:
- clarify the reporting timeframes for unlawful sexual contact and inappropriate sexual conduct incidents
- replace some references to ‘distress’ and ‘impact’ with ‘harm and/or discomfort’ to align with the legislation
- more clearly define ‘could reasonably have been expected to have caused’
- provide more guidance on the repeated use of restrictive practices.
We've also amended our Reportable incidents: Unlawful sexual contact or inappropriate sexual conduct fact sheet, Reportable incidents workflow, and the ‘Unlawful sexual contact or inappropriate sexual conduct’ incident in our SIRS decision support tool in line with the updates to the guidelines.
If you have any SIRS queries, you can call us on 1800 081 549 or send us an email at sirs@agedcarequality.gov.au.
Quality and safety in home services risks in focus: Organisational governance
As providers of home services, under the Aged Care Act 1997 you are responsible for the delivery of quality care and services to consumers and for ensuring that your organisation has effective governance, systems and processes in place to manage associated risks.
Through our analysis of complaints, performance assessments, compliance outcomes and other data sources, we have identified the 5 most common risks that can impact your ability to deliver high-quality care and services. These are outlined in our recently released ‘Quality and safety in home services – 5 key areas of risk’ resource. They are:
| Key areas of risk | What is the problem or risk to be addressed? |
|---|---|
| Organisational governance (Refer to Chapter 2) |
A lack of oversight or inadequate organisational governance means that providers are less able to identify deficiencies and continuously improve. |
| Care planning and assessment (Refer to Chapter 3) |
Failure to undertake appropriate assessment and care planning can deprive consumers of the care and services they need. |
| Clinical care (Refer to Chapter 4) |
Poor clinical governance can result in poor outcomes for consumers (even where clinical care is not being delivered). |
| Vulnerable consumers (Refer to Chapter 5) |
Failure to identify (and appropriately support and monitor) vulnerable consumers can lead to particularly poor outcomes for consumers who are already at risk. |
| Management of package funds (Refer to Chapter 6) |
Inappropriate use of Home Care Package funds or failure to consult with consumers regarding fees and charges can result in consumers receiving care and services that do not meet their assessed care needs. |
Over the next 5 editions of the Quality Bulletin, we will focus in more detail on each of the identified risks. This month’s first in-focus risk is Organisational governance.
What’s the problem?
A lack of oversight or inadequate organisational governance means that providers are less able to identify issues and opportunities for continuous improvement.
What has the Commission found?
Through the Commission’s quality assessment and monitoring activities between 1 January 2021 and 30 June 2022, 49% of home services providers who were assessed against Aged Care Quality Standard 8: Organisational governance were found to be non-compliant with one or more requirements of this standard.
What should home service providers consider when reviewing their performance?
1. How do you know that consumers receiving care and services through your sub-contracted organisations are actually receiving those services, and that those services are delivered in line with the requirements outlined in their care plans?
Where services are sub-contracted, as the provider you are still responsible for maintaining oversight of these contracted services. For example, if you do not have adequate oversight over a consumer’s clinical care delivery provided by a sub-contracted organisation, issues such as missed services or medication mismanagement may not be identified and actioned in a timely manner. This can then lead to poor quality of care and impact negatively on consumer outcomes.
2. What systems does your organisation have in place to identify and manage high-impact, high-prevalence risks and how are these systems reviewed to deliver improved outcomes for consumers?
Your organisation should have an effective information management system and processes that give members of your workforce access to training, support and information that help them in their roles. It is important for staff to identify and manage high-impact, high-prevalence risks to deliver improved outcomes for consumers. As appropriate to their role, staff (including management) should be able to access relevant information at any point in time on:
- any high-prevalence, high-impact risks to consumers across the service – these are common risks that can have a significant impact on the health, wellbeing and safety of consumers and may include falls, pressure injuries/wounds, choking, medication mismanagement, physical or cognitive decline
- consumers who have been involved in incidents and any strategies in place to manage risks to their health, safety and wellbeing
- consumers awaiting a higher level of Home Care Package or residential care.
3. How do you know that your organisation’s governance systems for managing and communicating information, managing finances, ensuring regulatory compliance, and managing feedback and complaints are effective?
Having effective governance systems is integral to ensuring your organisation delivers safe and quality care that meets the needs of consumers. You should consider what information is informing your understanding of whether these systems are operating effectively.
More information
Further information about these key risks and guidance for reviewing your performance are available in our ‘Quality and safety in home services – 5 key areas of risk’ resource.
Incident management system essential element #6 – Close the loop
An incident management system (IMS) is a critical feature of effective clinical governance for all aged care providers.
There are 6 essential elements to an effective IMS. In this final article in our series, we look at the sixth element that residential aged care and home care providers must demonstrate.
IMS essential element #6 – Close the loop
Closing the loop helps you to analyse and learn from incidents, which allows you to improve your IMS, reduce the risk of harm to consumers, and improve the overall quality and safety of the care you provide.
Analyse incident trends and data
Your IMS must enable you to collect data and other information about incidents so you can:
- identify and address systemic issues
- identify repeated occurrences (including alleged/suspected occurrences) of similar incidents or near misses
- analyse trends and identify patterns of incidents (for example, behaviours)
- provide feedback and training to your staff about preventing and managing incidents
- provide information to the Commission as requested.
Share lessons learned
Sharing what you learned from incidents with staff, management, consumers and family/representatives, those involved in the incident and others as needed is an important step to prevent recurrences.
Learning from incidents and near misses, understanding and communicating what can be done to prevent them and building trust are key aims of a good incident management process.
Improve your IMS
You need to consistently monitor your IMS and broader incident management processes to assess their effectiveness, reliability and opportunities for improvement.
Factors to consider include:
- the timeliness of your analysis (for example, how often you analyse your data)
- the implementation of actions (for example, whether the actions were completed)
- the effectiveness of the actions in reducing the recurrence of harm (for example, have you evaluated the outcomes of the actions)
- feedback from those affected by the incident
- sharing what was learned.
More information
Read our ‘Effective incident management systems: Best practice guidance’ for detailed information about how to develop and embed an IMS in your service.
You can read the previous articles in this series on our website.
We want to work with aged care consumers
The Commission is excited to establish a panel of people who use Australian government-funded aged care services, their carers and family members, and we’re currently accepting expressions of interest.
The Consumers and Families Panel will help us understand what is important to older people receiving aged care services so we can improve how we regulate services and make sure the information we publish is useful and easy to understand.
We are inviting expressions of interest from people who are:
- currently living in residential aged care
- receiving aged care services at home or in the community
- considering accessing aged care services in the next 12 months
- a carer, supporter or close family member of a person who currently receives aged care services.
We want the panel to reflect the diversity of people accessing aged care including people who live with dementia or disability, as well as First Nations people, people from culturally and linguistically diverse backgrounds, and lesbian, gay, bisexual, trans/transgender, intersex, queer and other sexuality, gender, and bodily diverse people.
Once the panel is established, we will invite members to share their ideas and opinions about issues such as:
- what is of most concern to people receiving care that we should know about
- how people can be better supported to interact with us
- how we can reach people better
- new flyers, videos or other resources we develop.
Panel members will be able to provide input in different ways, including by email or telephone or taking part in online or in-person meetings.
Please share this information with your residents or people receiving your services, encouraging them to join our panel if they are interested.
Anyone interested in applying for the Consumers and Families Panel can register via our website or by calling 1800 951 822.
Online learning platform (Alis) – free access trial and upgrades
The Commission is committed to supporting aged care providers and workers with access to educational content anywhere and at any time. We’re now providing wider access to Alis, our Aged Care Learning Information Solution, and we recently upgraded the platform to improve the learning experience for the sector.
Alis access for sector workers
We are trialling expanded free access to Alis. From 1 July 2022, all workers of Commonwealth-funded aged care providers can access our learning content free of charge.
Workers can sign themselves up to Alis at learning.agedcarequality.gov.au. When signing up, workers need to link their account to the service provider they work for and be approved by the administrator for their service.
Learning managers and administrators at aged care services can also sign up their staff and provide them with access to Alis content.
Look and feel changes
If you’re an existing Alis user, you’ll notice that we’ve made some improvements to the look and feel of the platform as part of our upgrade, including your dashboard.
Even though your dashboard looks different, the content remains the same as part of this upgrade. This means that you can still access reporting and insights about learning just like you did before.
Get your service ready
We will be rolling out new, engaging learning content over the next 12 months to help leaders and staff understand their responsibility to deliver safe, quality care.
If you are a learning manager or administrator at a Commonwealth-funded aged care provider and you would like to find out more about accessing Alis, please complete the expression of interest form on the Commission’s website. Once your service has been added to the Alis platform, you will be able to provide access for your learners either individually or via a bulk upload process.
If your service already has access to the Alis platform, you can email us at education@agedcarequality.gov.au to check or update the administrator for your service. This will ensure that your service is able to give your workers access to our free online learning content.
Our approved provider application fees have been updated
In November 2021, following a consultation process, we introduced fees and charges for approved provider applications.
Every year, the Commission is required to review the charging model and fees ahead of the new financial year.
We recently released our 2022–23 Cost Recovery Implementation Statement (CRIS), which outlines the fees, charges and waivers that apply to:
- organisations seeking approved provider status
- existing approved providers seeking approval to provide additional services or change their services.
There is a small reduction in fees in 2022–23 due to a decrease in staffing costs and a minor increase in licensing costs for the Commission. The new fees took effect on 1 July 2022.
The old and new fees are included in the CRIS, as is information on the indexed fees and forward financial estimates of revenue and expenses.
New and updated Commission resources
- New: How prepared are you for a COVID-19 outbreak? fact sheet
- New: Clinical alert – Be on guard against another wave of COVID-19 infections (July 2022)
- Updated: We’ve updated our Monitoring performance workshop to introduce a more risk-focused lens to assist providers to identify and understand key risks in the home services sector. This includes references to content in the recently released ‘Quality and safety in home services – 5 key areas of risk guidance’.
- Updated: We’re continuing to improve our operational efficiency and strengthen our regulatory capability. In August we’ll be updating our Assessment Team and Performance Reports to focus more on presenting overall findings and consumer outcomes. We use these reports for site and quality audits and assessment contacts. Following an onsite visit, we’ll send you a survey so you can give us your feedback on the revised reports. More information on our quality assessment activities is available in our Regulatory Bulletins.
Other resources
- The Older Persons Advocacy Network (OPAN) held an online national forum on 30 June ‘Getting ready to listen – service provider perspectives’. In the forum, providers and advocates shared their perspectives on why being ready to listen matters when it comes to sexual assault disclosures in residential aged care. The #ReadyToListen project was launched to improve responses to – and prevent – sexual assault in residential aged care. A recording of this forum is now available.
- Throughout August 2022, the Australian Psychological Society will continue to offer 2 free online mental health courses for health professionals working in residential aged care facilities. The Applied mental health in residential aged care: Practical program for clinicians is designed for psychologists, psychiatrists, social workers, occupational therapists, mental health nurses, and Aboriginal and Torres Strait Islander health workers. The Supporting the mental health of older people in residential aged care: Mental health awareness training course is available for non-mental health trained workers in residential aged care, for example registered nurses, physiotherapists, audiologists, speech pathologists, dieticians, personal care workers, attendants and peer workers. Both courses are funded by the Department of Health and Aged Care and carry Continuing Professional Development (CPD) credits.