The Quality Standards Resource Centre helps extend understanding of the strengthened Aged Care Quality Standards, which take effect from 1 November 2025. The Resource Centre will be updated to reflect key changes made to the draft strengthened Standards. You can search for resources by using keywords, or filtering by standard, outcome, audience and theme. Before using the Resource Centre, please read the terms of use.
Communication at clinical handover
This resource focuses on structured clinical handover processes to improve communication during patient care transitions. It highlights the importance of standardising handover procedures to make sure relevant information is effectively communicated, reducing errors and enhancing patient safety, especially during care transfers in healthcare settings, including aged care.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.
Communicating for Safety
This resource provides tools and guidance on improving clinical communication to enhance patient safety. It focuses on key communication touchpoints, such as handovers, decision-making, and care transitions. Designed to support healthcare providers, it offers practical strategies to reduce errors and improve outcomes in aged care and other healthcare settings.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.
Code of Conduct for Aged Care
This resource outlines the Code of Conduct for Aged Care, which sets expectations for the behaviour of providers, governing persons, and workers. It promotes respect, safety, and quality in aged care services, ensuring people’s rights are protected. The Code includes guidance on handling concerns and preventing abuse or neglect.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.

Code of Conduct for workers
This resource outlines the Code of Conduct for Aged Care workers, detailing expected behaviours such as respect, honesty, and integrity. It ensures people receiving care are treated with dignity, kept safe from harm, and supported. The Code applies to all aged care workers, including volunteers.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.
Improving aged care with speech pathology: Why it matters and how it helps
This page highlights the role of speech pathologists in supporting older people with communication, eating, drinking, and swallowing difficulties. It provides resources for aged care providers on how to improve care quality through effective communication tools and tailored strategies. This resource includes practical examples, like sample plates and picture boards, for enhancing dining experiences and supporting individual choice.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.
Respecting the privacy and dignity of clients
This resource provides guidance about respecting the privacy and dignity of clients. It includes information about personal privacy, the Privacy Act, what classifies as health information, consent and privacy of information. It also includes information about person-centred care and client dignity.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.
Privacy and confidentiality – Introduction to aged care video
This resource is a training video guiding aged care staff on the importance of maintaining privacy and confidentiality for people receiving care. It covers protecting personal information, proper handling of sensitive data, and safe sharing practices, aiming to make sure clients feel secure in sharing information.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.

Partnerships in Care Agreement – Sample
This resource is a sample of what a partner agreement might look like. It can be used as a template. This document has been created to support aged care providers and individuals where all parties would like to put an agreement in place.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.

National Consensus Statement - Essential elements for recognising and responding to acute physical deterioration
This consensus statement outlines essential elements for recognising and responding to acute physiological deterioration in healthcare settings. It covers clinical processes like vital signs monitoring, diagnosis, and rapid response systems, as well as organisational aspects such as leadership, education, and evaluation. It provides generic information that can be applied to the aged care setting.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.

National framework for advance care planning documents
This resource provides a nationally consistent framework for advance care planning documents in Australia. It outlines principles, ethical considerations, and best practices for creating, implementing, and accessing advance care plans, including Advance Care Directives. It aims to guide policymakers, administrators, and healthcare providers in recognising people’s values, preferences, and rights regarding future care.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.

How to support everyday decision-making for people living with dementia in residential aged care: A guide for care workers
This guide offers practical strategies for care workers to support people with dementia in making everyday decisions within residential aged care settings. It covers communication techniques, promoting choice in personal care and daily activities, understanding body language, and emphasises person-centred care while respecting residents' preferences, dignity, and rights.
Allied health regulation
This resource provides information about the regulation of allied health professions in Australia. It includes those registered under the National Registration and Accreditation Scheme (NRAS) and self-regulating professions managed by professional peak bodies. It also provides links to further information about allied health professions currently registered with AHPRA and information for overseas-qualified practitioners.

Mental health and wellbeing - Suicidal thoughts and self-harm
This resource examines suicidal thoughts and self-harm in older adults, particularly in residential aged care. It discusses associated risk factors, the prevalence of mental health conditions, what organisations and individuals can do and gaps in understanding suicide risk. It also reviews interventions, highlighting the need for mental health assessments and training to improve detection and care.
Mental health and wellbeing - Screening tools
This resource covers screening tools for detecting anxiety and depression in older adults, especially in residential aged care. It discusses the importance of mental health screening, steps individuals and organisations can take, choosing appropriate tools, and highlights tools such as the Geriatric Depression Scale and Cornell Scale for Depression in Dementia. It emphasises early detection and routine mental health screening in aged care.
About speech pathologists - Aged care
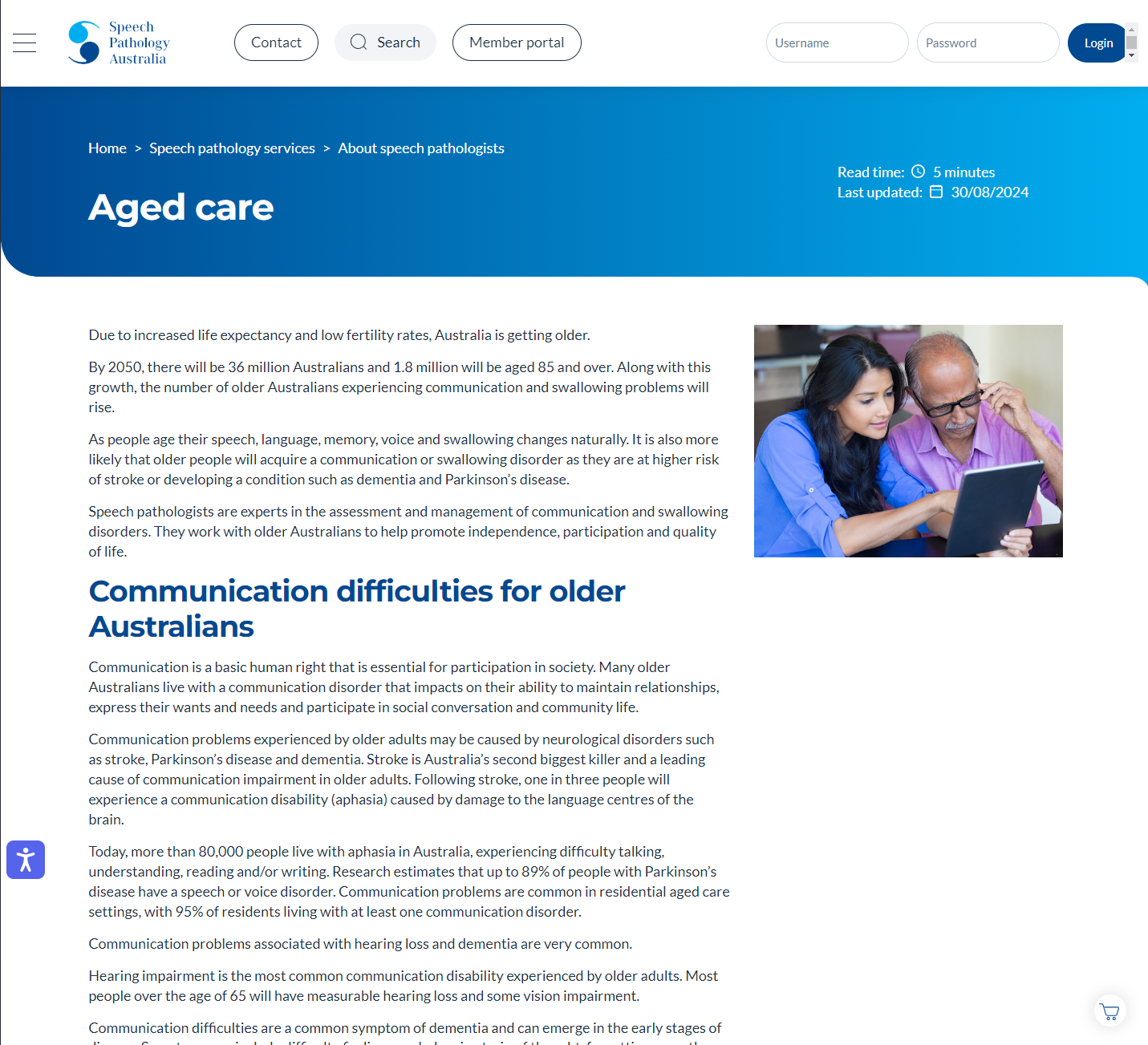
This resource discusses the role of speech pathologists in supporting older people with communication and swallowing disorders caused by ageing, neurological conditions, and other health factors. It highlights the prevalence of communication and swallowing difficulties in aged care, their impacts, and how speech pathology services promote independence, participation, and quality of life through assessment, therapy, and tailored interventions.
RACGP aged care clinical guide (Silver Book) - Part A - Multimorbidity
This resource provides guidelines for managing patients with multimorbidity in aged care settings. It includes frameworks for assessing treatment burden, identifying patients at risk, and developing individualised care plans. It recommends validated tools for screening, a focus on quality of life, and strategies for medication review and care coordination.

Mental health and wellbeing - Anxiety
This resource provides information on anxiety among older adults, especially those in residential aged care. It outlines risk factors, detection tools, and effectiveness of non-pharmacological interventions such as reminiscence therapy and cognitive behavioural therapy. It also provides guidance on what both individuals and organisations can do to prevent and manage anxiety effectively.
Mental health and wellbeing - Depression
This resource provides information on depression in older adults, particularly in residential aged care. It discusses risk factors, detection tools, and treatment approaches, including psychotherapy, music-based interventions, and exercise. It also provides guidance on what both individuals and organisations can do to prevent and manage depression effectively.
RACGP aged care clinical guide (Silver Book) - Part B - Physiology of ageing
This guide reviews the physiological changes associated with ageing across multiple body systems, including cardiovascular, nervous, renal, respiratory, gastrointestinal, immune, skin, haematological, endocrine, and musculoskeletal systems. It also discusses clinical manifestations of these changes, implications for care, and provides recommendations for adjusting clinical practice to meet the needs of older adults, including medication reviews, hydration, mobility support, and preventive health strategies.

RACGP aged care clinical guide (Silver Book) - Part B - Geriatric syndromes
This guide outlines the challenges of diagnosing and managing geriatric syndromes, describing clusters like immobility, instability, incontinence, frailty, sarcopenia, and cognitive impairment. It introduces the 'Geriatric 5Ms' framework: Mind, Mobility, Medications, Mult complexity, and Matters Most, which assists in comprehensive assessment and care planning for older adults, focusing on mental health, physical function, medication review, complex health needs, and care goals.








