The Quality Standards Resource Centre helps extend understanding of the strengthened Aged Care Quality Standards, which took effect from 1 November 2025. You can search for resources by using keywords, or filtering by standard, outcome and audience. Before using the Resource Centre, please read the terms of use.
Program of Experience in the Palliative Approach (PEPA)
This page provides resources about palliative care for health professionals. The education resources support placement and workshop learning, but can be used for self-directed learning.
End-of-life care - Last days of life
This resource provides guidance on end-of-life care during the last days of life, relevant for aged care settings. It focuses on maintaining comfort, managing symptoms, and reducing unnecessary interventions. Clinicians are supported in offering compassionate care, addressing potential emergencies, and involving family members while ensuring that older people are treated with dignity during their final days.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.

Informed consent - Health Direct
This resource explains the legal requirements and processes for obtaining informed consent for medical treatments, procedures, and care. It is relevant to aged care by ensuring that people understand their healthcare options, risks, and benefits, supporting their ability to make informed decisions about their health and wellbeing.
Pharmaceutical Benefits Scheme (PBS) medication chart maximum duration in residential aged care
This resource outlines the Pharmaceutical Benefits Scheme (PBS) medication chart's maximum duration in residential aged care. It explains the use of both paper-based and electronic National Residential Medication Charts (NRMC), highlighting their role in managing prescriptions, medication supply, and administration. The document provides guidance on compliance, chart expiry, and medication safety within aged care facilities.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.

Medication management for health practitioners
This resource supports health practitioners in managing medicines through the use of medication charts in aged care facilities and hospitals. It provides guidelines for safe prescribing, administration, and communication. The resource includes both paper-based and electronic medication chart systems to reduce errors, improve patient safety, and streamline medication management processes in aged care settings.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.
Electronic prescribing
This resource outlines the framework for electronic prescribing, offering an alternative to paper prescriptions for healthcare providers and consumers. It explains the benefits of electronic prescriptions, such as reducing errors, improving efficiency, and supporting medication safety. The resource also covers technical and legislative requirements for implementing electronic prescriptions in various healthcare settings.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.
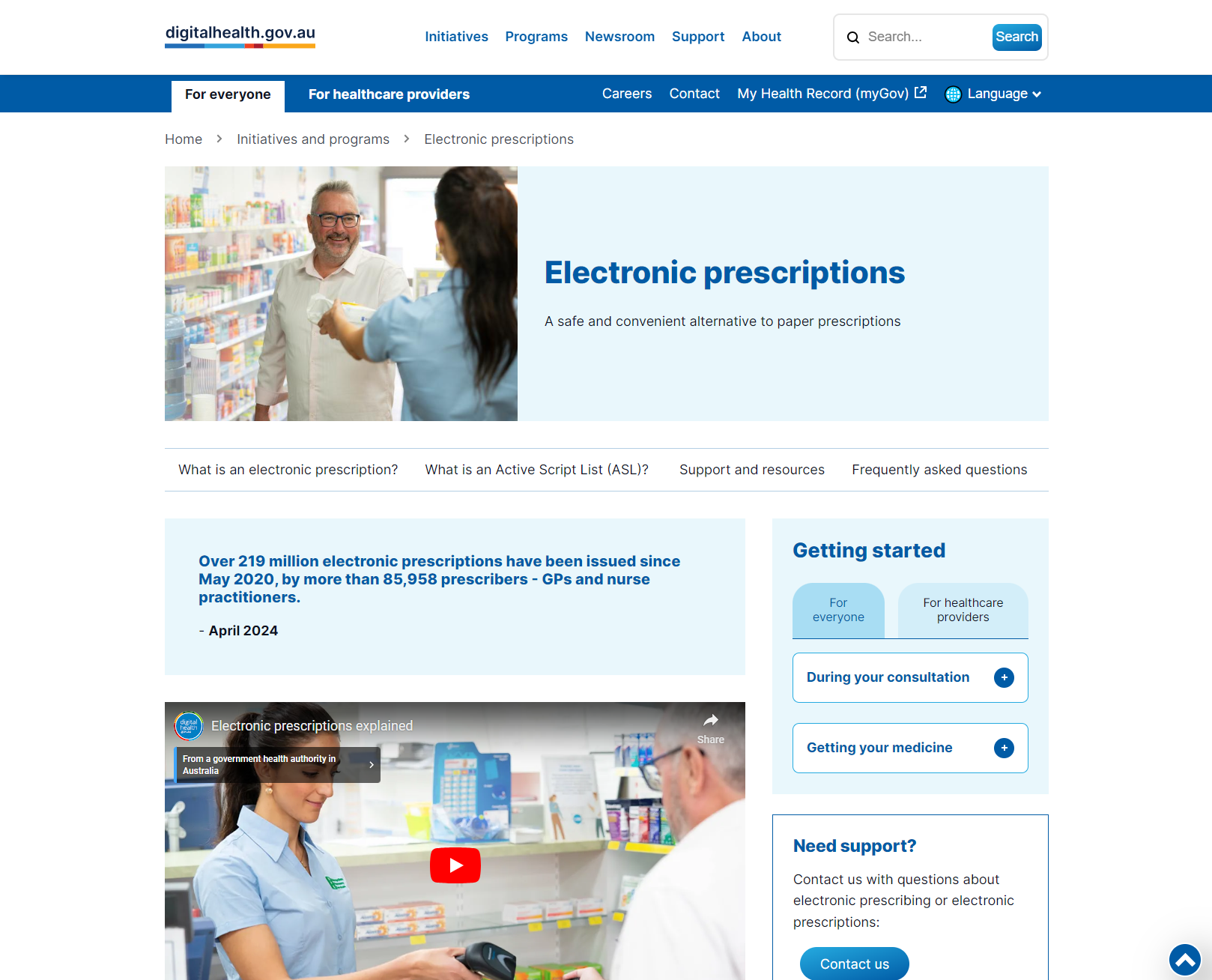
Electronic prescriptions
This resource provides an overview of electronic prescriptions, which offer a digital alternative to paper prescriptions. It explains how electronic prescriptions can be issued by healthcare providers and stored on digital devices for convenience. The resource also details the benefits of the Active Script List (ASL) for managing multiple prescriptions, enhancing efficiency and medicine safety.
Palliative care education and training
This resource provides information on free palliative care education programs available for health and aged care workers. It includes details about various training opportunities, such as online courses and in-person sessions, designed to enhance skills in delivering high-quality palliative care. The programs cover key topics like symptom management, communication, and multidisciplinary care. This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.

QI Program quick reference guide – Unplanned weight loss
This resource provides a quick reference guide for approved aged care providers on collecting and reporting data related to unplanned weight loss as part of the National Aged Care Mandatory Quality Indicator Program. It outlines reporting requirements for significant and consecutive unplanned weight loss and offers guidance on how to track and submit data quarterly. This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.

Digital Health Developer Portal - Aged Care Clinical Information System Standards v1.0
This resource outlines the Aged Care Clinical Information System (ACCIS) Standards version 1.0, which sets minimum software requirements for clinical information and electronic medication management systems in aged care. The standards support interoperability, data sharing, and improved care quality by enabling safe and efficient clinical decision-making and information exchange between care providers.
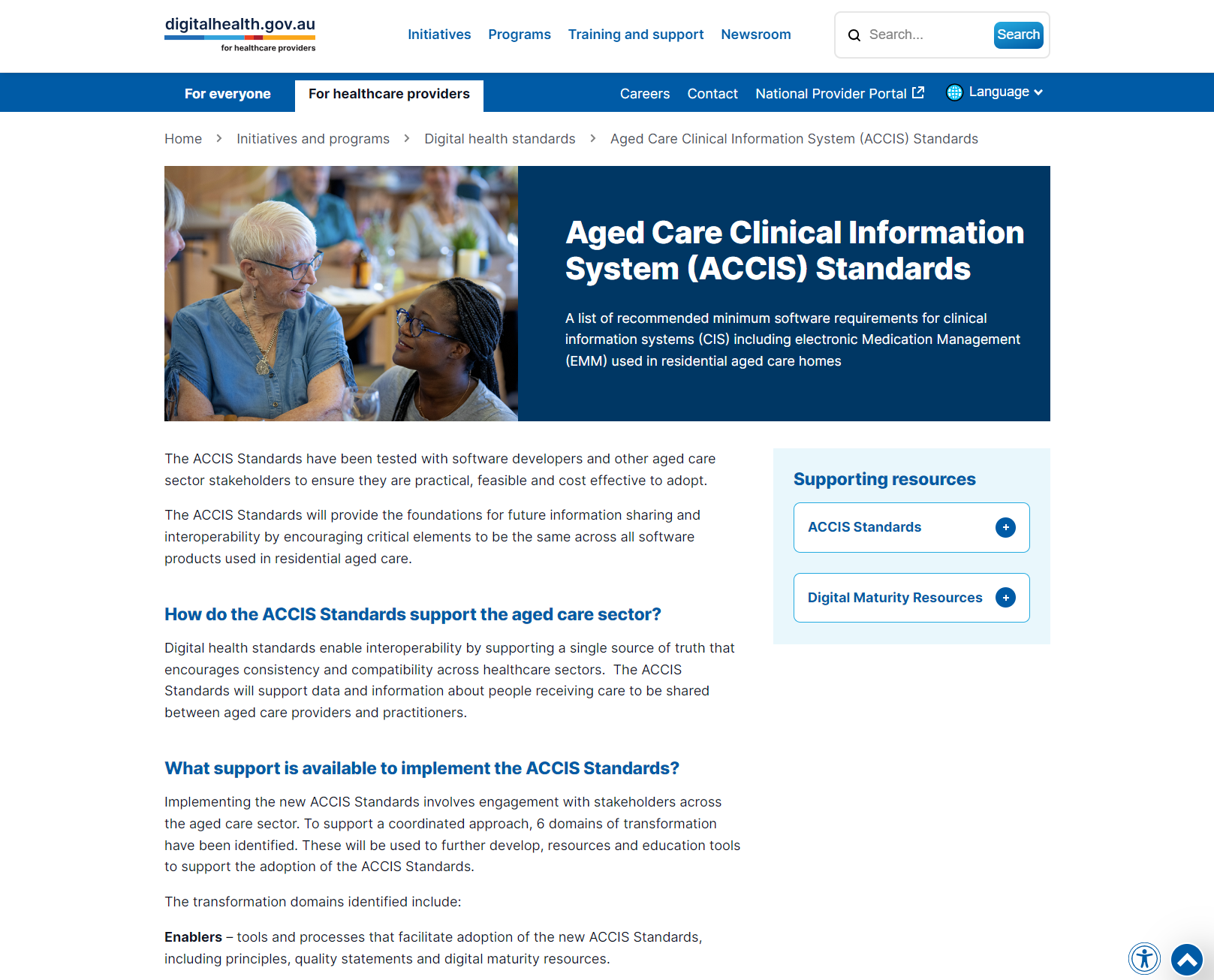
Aged Care Clinical Information System (ACCIS) Standards
This resource outlines the Aged Care Clinical Information System (ACCIS) Standards, providing minimum software requirements for clinical information systems used in aged care. It supports interoperability, data sharing, and safe clinical decision-making. The standards aim to enhance care coordination, improve data accuracy, and ensure compliance with privacy and security protocols within residential aged care settings.
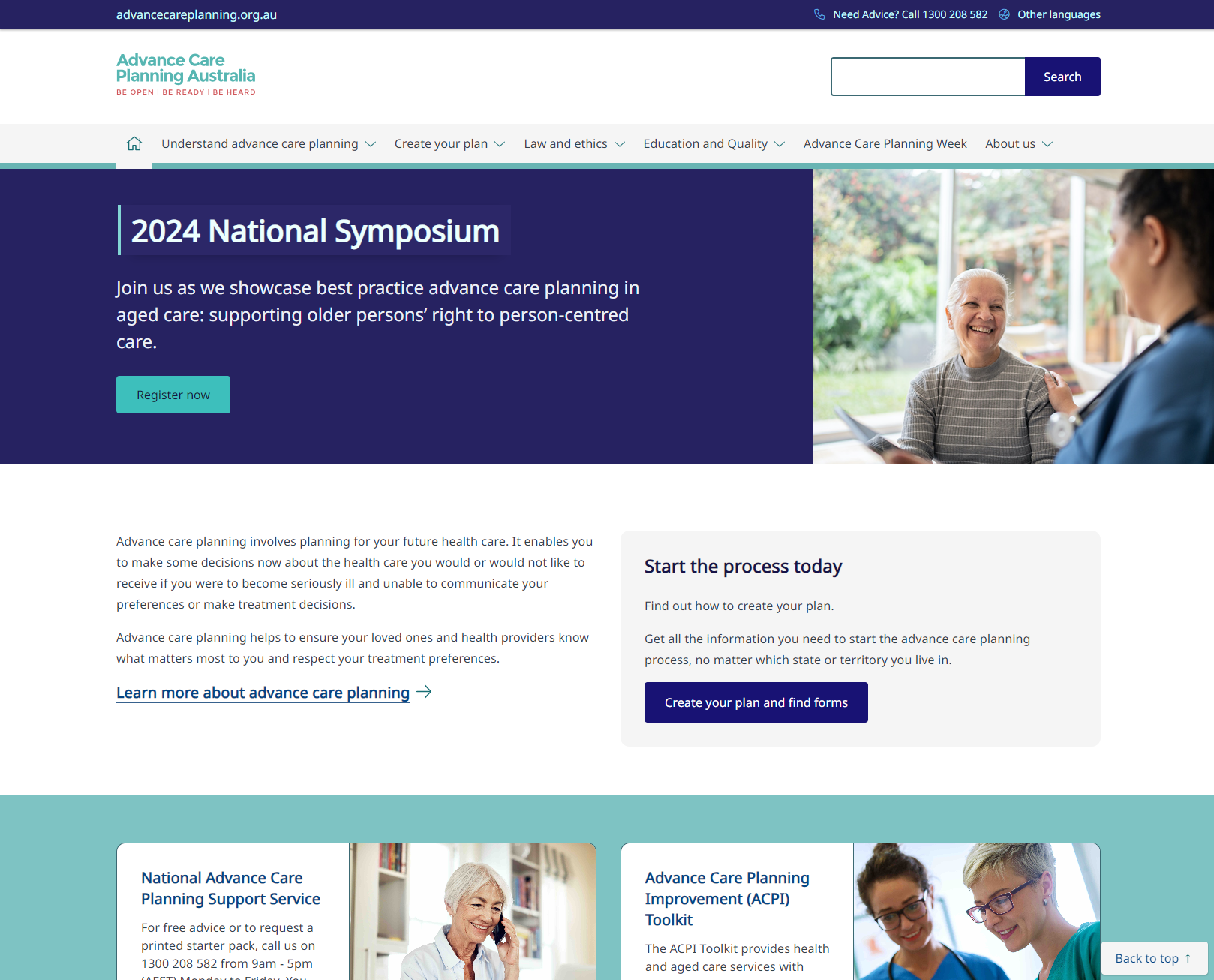
Advance Care Planning Australia
This resource provides information on advance care planning, which enables people to make decisions about their future health care in case they are unable to communicate their preferences. It helps ensure that healthcare providers and loved ones understand and respect their treatment choices. The resource includes tools, forms, and advice for creating an advance care plan.
The A-PRECISE model: Building capacity to prevent and manage infections in residential aged care
The A-PRECISE model (Australia – PReventing infECtions In reSidential agEd care) is an infection prevention strategy co-designed with residents, family members and staff in residential aged care homes. The model provides clear and actionable strategies for creating an environment where effective infection prevention and control (IPC) practices can thrive.





