The Quality Standards Resource Centre helps extend understanding of the strengthened Aged Care Quality Standards, which took effect from 1 November 2025. You can search for resources by using keywords, or filtering by standard, outcome and audience. Before using the Resource Centre, please read the terms of use.
Positive ageing
This resource focuses on positive ageing, encouraging older people to maintain their health, independence, and connection to community. It covers planning for healthy ageing, staying physically active, and accessing aged care services when needed. The resource promotes ageing as a positive experience, offering practical guidance to support older people in living well. This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.
Monthly Care Statements for residential aged care
This resource provides information about Monthly Care Statements, including why they are important, who can give them, and the benefits for residents and providers.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.
Physical activity and exercise guidelines - For older Australians (65 years and over)
This resource provides Australia’s physical activity and sedentary behaviour guidelines for older adults. It outlines how much physical activity is recommended, the importance of reducing sitting time, and the benefits of staying active. The guidelines help promote better physical and mental health across the lifespan.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.
Partners in Culturally Appropriate Care (PICAC)
This resource supports aged care providers in delivering culturally appropriate care for people from culturally and linguistically diverse (CALD) backgrounds. It offers free training, workshops, and resources, helping providers understand and respect diverse needs, ensuring safe, inclusive, and culturally responsive care across all settings.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.
National framework for advance care planning documents
This resource provides a nationally consistent framework for advance care planning documents in Australia. It outlines principles, ethical considerations, and best practices for creating, implementing, and accessing advance care plans, including Advance Care Directives. It aims to guide policymakers, administrators, and healthcare providers in recognising people’s values, preferences, and rights regarding future care.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.

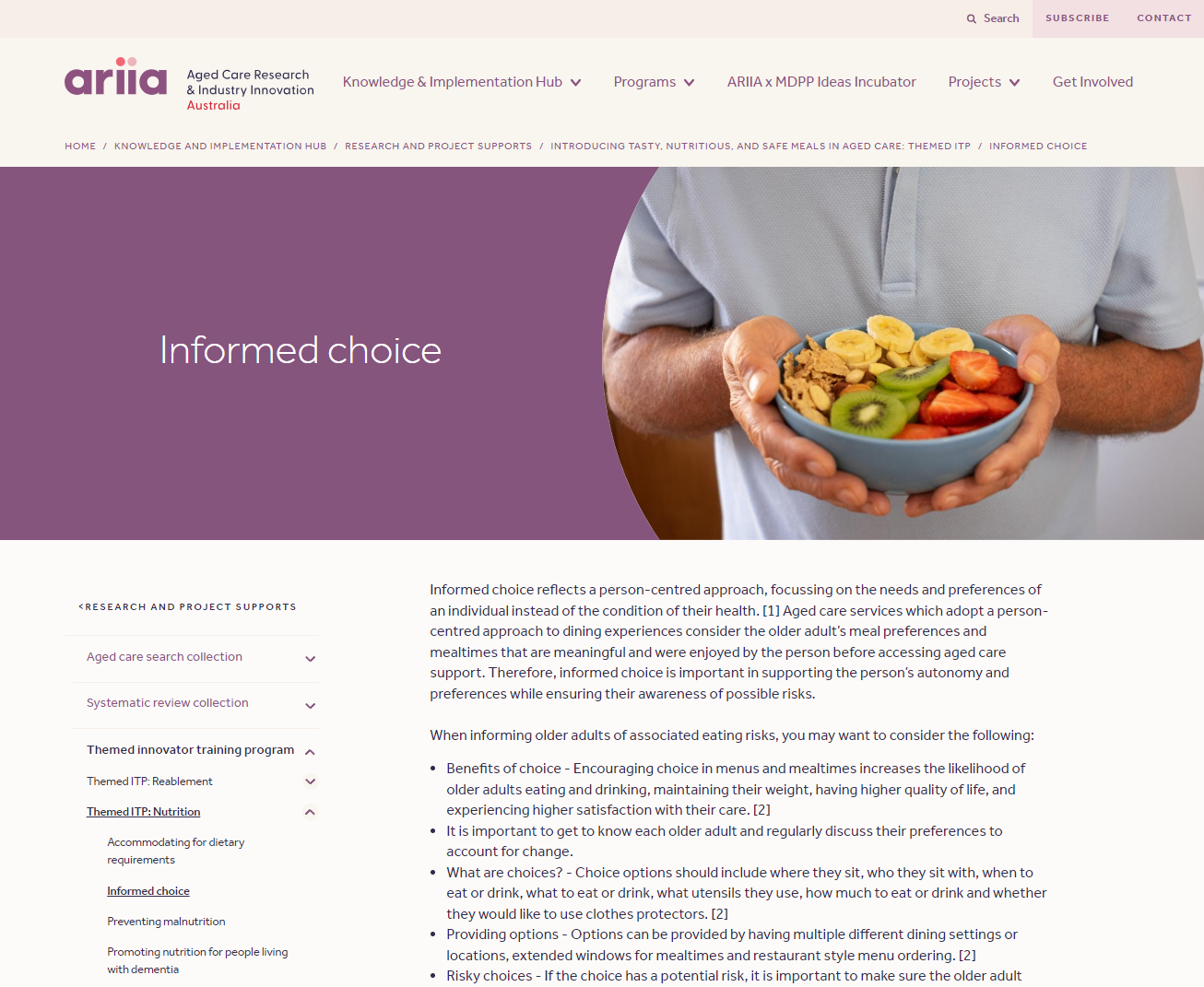
Nutrition - Informed choice
This resource discusses the importance of informed choice in aged care dining, emphasising a person-centred approach. It highlights the benefits of offering choice in meals and mealtimes, outlines how to manage decisions that involve risk, and provides tools for aged care workers to support resident autonomy while ensuring safety and satisfaction.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.
Nourishing connections: The vital role of social dining in aged care
This resource explains how social dining in aged care can enhance nutrition and wellbeing by fostering social connections. It encourages creating positive dining environments that promote engagement and respect personal preferences during mealtimes.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.

Food and dining - your choices matter
This fact sheet informs aged care residents of their rights to safe, enjoyable, and respectful dining experiences. It outlines steps for raising concerns with providers about food and dining, offers a preference form for residents to communicate their dietary needs, and provides contact information for support services if issues remain unresolved. This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.

Support at Home program handbook
This resource outlines the design and key components of the Support at Home program, effective from 1 November 2025. It provides guidance for aged care providers on service delivery, budgeting, and assessment processes, helping older people remain independent at home. It also details regulatory requirements and transition from existing programs.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.

Supporting Better Communication & Care
This webpage provides resources to help improve communication, care and support for people who are deaf, Deaf, hard of hearing, or who experience hearing loss. It includes 3 tools: Everyday Communication, Inclusive Healthcare, and Building Competency. There are also links to other relevant resources.

Case study - Safe and Appropriate use of Psychotropic Medicines - Residential Aged Care
This resource is a fictional scenario that follows an older person’s care pathway with a residential aged care provider. The resource focuses on the systems and processes to support high-quality care of older people living with cognitive impairment. It includes 4 key priority areas: person-centred care, medication management, managing changed behaviours and transitions of care.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.

Case study - Safe and Appropriate use of Psychotropic Medicines - In-home Aged Care
This resource is a fictional scenario that follows an older person’s care pathway with an in-home aged care provider. The resource focuses on the systems and processes to support high-quality care of older people living with dementia. It includes 4 key priority areas: person-centred care, medication management, managing changed behaviours and transitions of care.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.

Safe and appropriate use of psychotropic medicines for aged care - Fact sheet
This fact sheet is informed by the Psychotropic Medicines in Cognitive Disability or Impairment Clinical Care Standard (CCS), developed by the Australian Commission on Safety and Quality in Health Care. The CCS describes the safe and appropriate use of psychotropic medicines for people with cognitive disability or impairment, in a way that upholds their rights, dignity, health and quality of life.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.

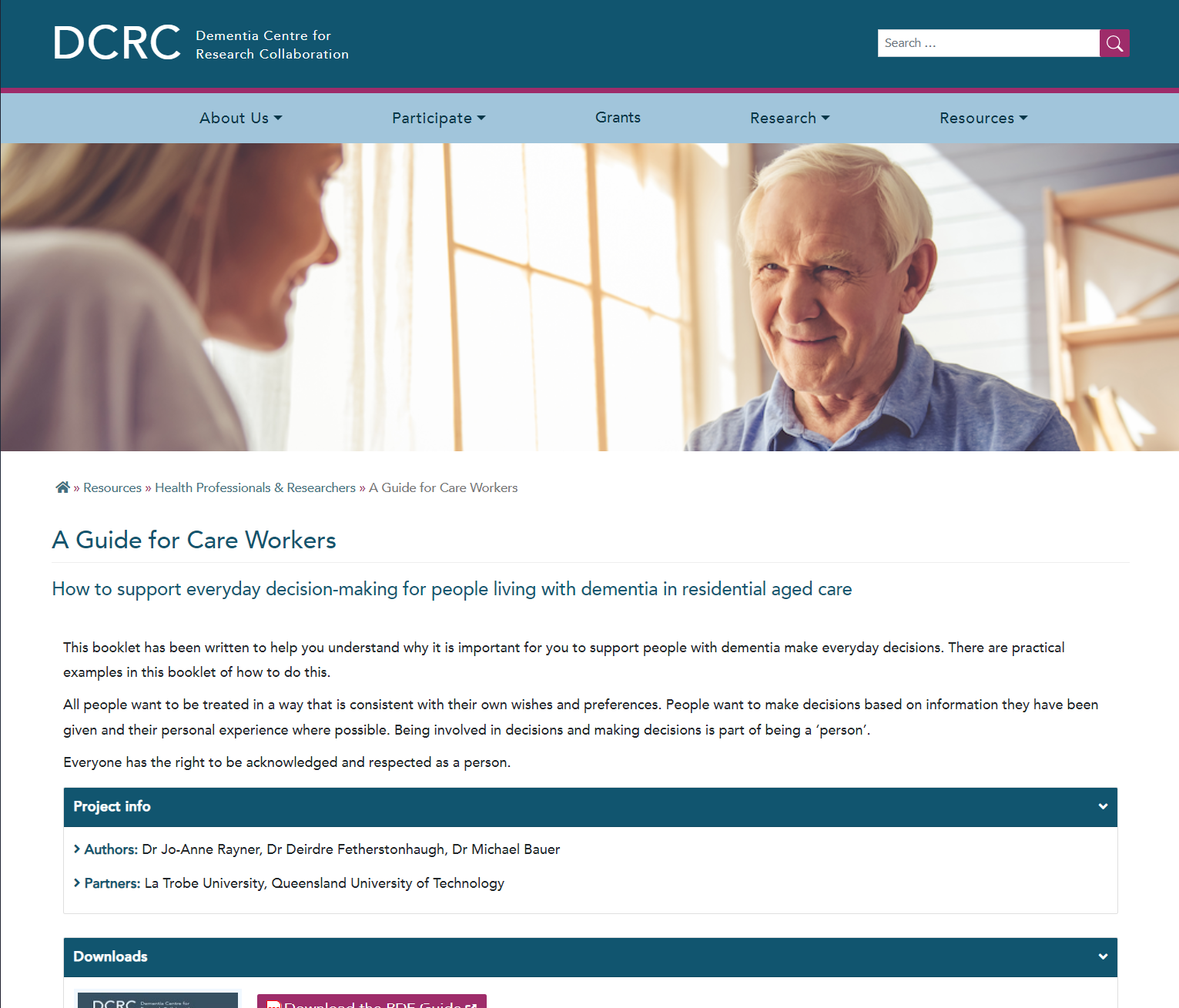
How to support everyday decision-making for people living with dementia in residential aged care: A guide for care workers
This guide offers practical strategies for care workers to support people with dementia in making everyday decisions within residential aged care settings. It covers communication techniques, promoting choice in personal care and daily activities, understanding body language, and emphasises person-centred care while respecting residents' preferences, dignity, and rights.
RACGP aged care clinical guide (Silver Book) - Part A - Behavioural and psychological symptoms of dementia
This guide offers principles and practice points for assessing and managing behavioural and psychological symptoms of dementia (BPSD) in aged care. It includes frameworks for comprehensive patient assessment, non-pharmacological and pharmacological interventions, medication review, and personalised care plans to improve care outcomes for dementia patients.

RACGP aged care clinical guide (Silver Book) - Part A - Dementia
This resource offers guidance on diagnosing and managing dementia, covering its impact on cognitive and physical functions, screening methods, and differential diagnoses. It discusses appropriate use of medications, non-pharmacological approaches, and ongoing care plans for supporting those with dementia. It includes practical recommendations on cognitive assessments, functional reviews, and medication management.

RACGP aged care clinical guide (Silver Book) - Part B - Multiculturalism in aged care
This guide discusses multiculturalism in aged care, addressing the diverse needs of culturally and linguistically diverse (CALD) older adults. It covers healthcare principles, communication strategies, clinical considerations, and culturally tailored approaches for areas like medication management, dementia, mental health, nutrition, and substance use. It also provides practical advice for general practitioners, carers, and aged care facilities to deliver culturally safe and effective care.

RACGP aged care clinical guide (Silver Book) - Part B - Older Aboriginal and Torres Strait Islander people
This guide addresses barriers faced by Aboriginal and Torres Strait Islander peoples in accessing aged care, such as cultural safety, geographic challenges, and geriatric syndromes experienced at younger ages. It discusses the importance of culturally appropriate care, the use of specific assessment tools, and the unique needs of the Stolen Generation within residential and community settings.

RACGP aged care clinical guide (Silver Book) - Part B - Supporting independent living in older people
This guide discusses strategies for supporting independent living in older adults, covering concepts of healthy ageing, using aged care services, respite care, and re-aligning function. It highlights the role of general practitioners in promoting autonomy, addressing individual needs, and avoiding ageist language while facilitating access to community or residential care services.

RACGP aged care clinical guide (Silver Book) - Part B - Disability in aged care
This guide addresses the management of disabilities in older adults, including mobility, cognitive impairments, developmental disabilities, hearing and visual impairment, psychiatric conditions, and neurodegenerative disorders. It outlines approaches for general practitioners to provide holistic care, monitor health risks, adapt support systems, and coordinate with allied health professionals in residential aged care settings.






