The Quality Standards Resource Centre helps extend understanding of the strengthened Aged Care Quality Standards, which took effect from 1 November 2025. You can search for resources by using keywords, or filtering by standard, outcome and audience. Before using the Resource Centre, please read the terms of use.
RACGP aged care clinical guide (Silver Book) - Part B - Older people in rural and remote communities
This guide discusses providing aged care in rural and remote communities, focusing on the unique needs of older residents, the role of GPs in care coordination, and overcoming challenges like limited services and workforce shortages. It covers building telehealth connections, establishing collaborative care models, and offers a checklist for newly arrived GPs to support quality care for older adults.

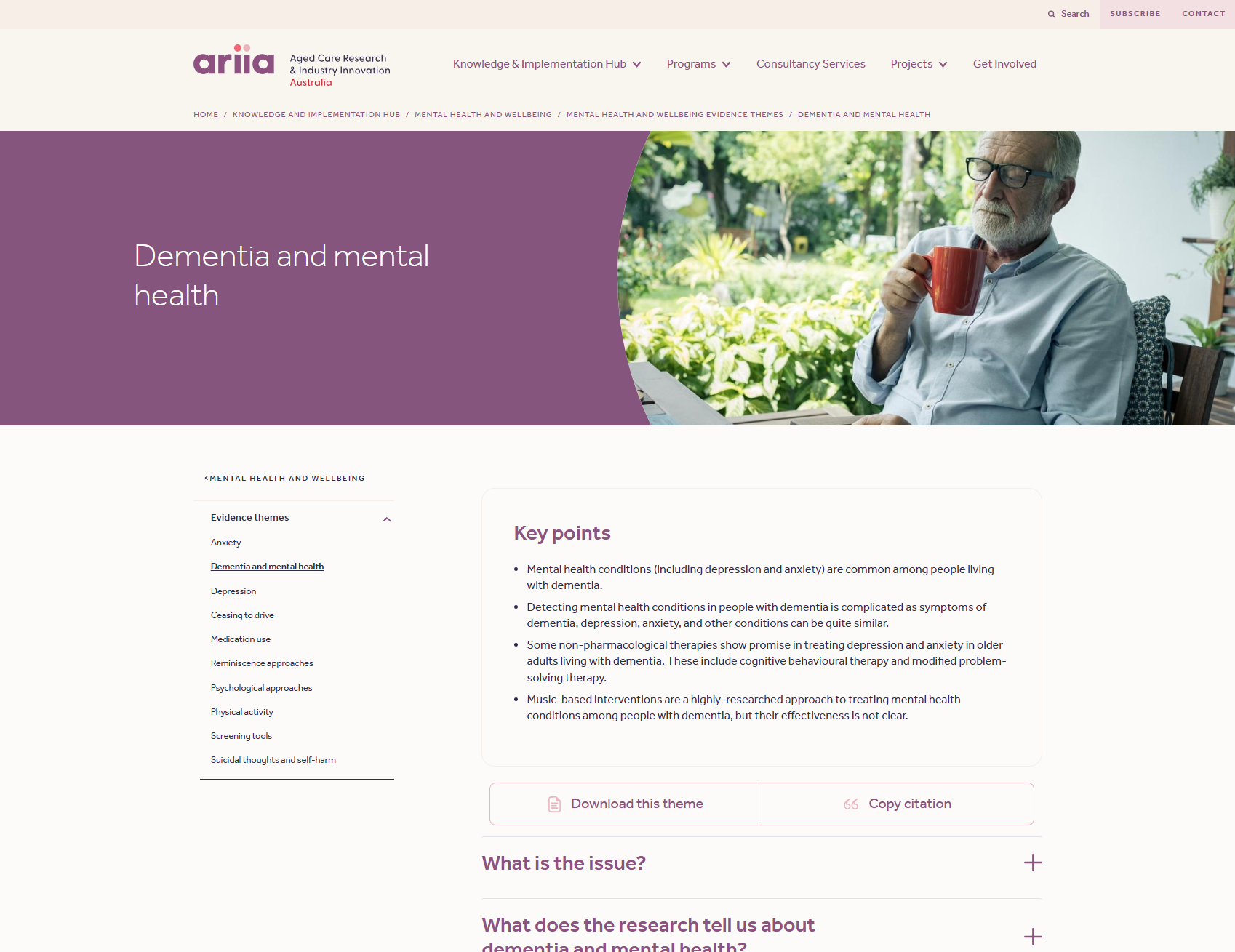
Mental health and wellbeing - Dementia and mental health
This resource examines mental health challenges in people living with dementia, covering complexities in diagnosing conditions like depression and anxiety. It provides evidence-based insights on therapeutic approaches, including music and cognitive therapies, and offers tools to aid aged care providers in supporting mental health in dementia care.
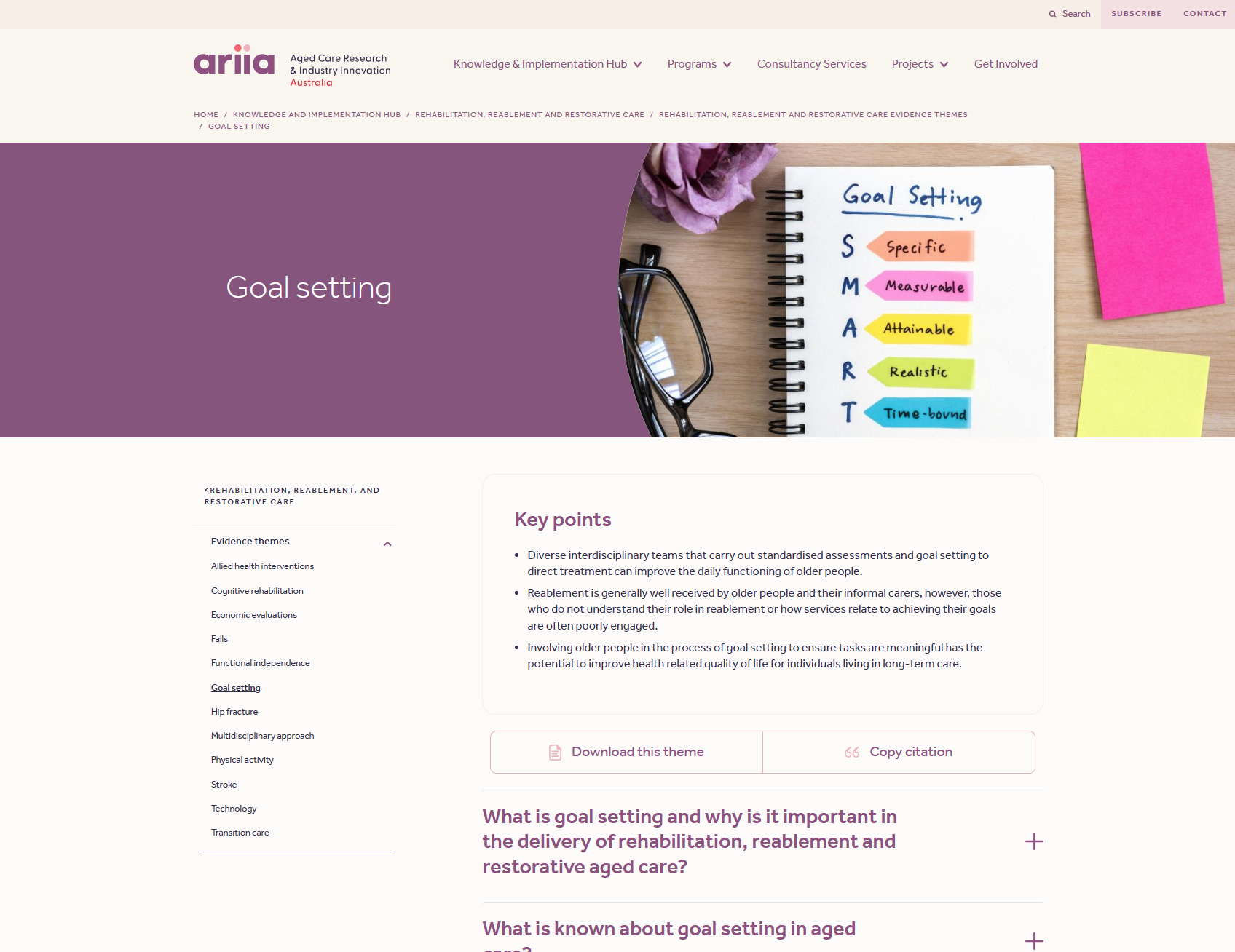
Goal setting
This resource discusses the role of goal setting in enhancing rehabilitation, reablement, and restorative care for older people. It highlights the value of involving older people in defining goals and the positive impact of goal setting on engagement, daily function, and quality of life.
First Nations - YouTube videos
This resource includes a series of YouTube videos developed by the Aged Care Quality and Safety Commission. Australian First Nations older people discuss good quality, culturally appropriate and safe aged care, including person-centred care, rights and how to speak up about care. This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.

Food and drink in your aged care - supporting informed choice and risk - staff poster
This resource provides guidance for aged care staff on supporting older people's informed choices regarding food and drink, even when those choices involve personal risks. It encourages staff to respect resident autonomy, provide information on risks, document decisions, and ensure access to professional advice, promoting dignity and quality of life in care settings. This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.

Creating behaviour support plans that better support residents
This document outlines the development of behaviour support plans (BSPs) in aged care, focusing on person-centred assessments, identification of triggers, tailored strategies, and regular reviews. It highlights the involvement of healthcare professionals and adherence to care principles to effectively manage residents’ behavioural changes and improve their quality of life.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.
Restrictive practices provider resources
This resource offers guidance and tools for aged care providers on managing restrictive practices. It emphasises using restrictive practices as a last resort, obtaining informed consent, and developing behaviour support plans. The materials include fact sheets, regulatory updates, webinars, and decision-making tools to ensure compliance with legislation and promote person-centred care.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.
Goal planning tool
This resource is a goal planning tool designed to support aged care providers in improving food, dining, nutrition, and consumer choice. It helps providers set objectives, track progress, and implement actions to enhance service quality, ensuring that people’s preferences and dietary needs are consistently met.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.

First Nations - Digital Flipchart - Your rights in aged care
A visual guide for conversations between providers/workers and older people about aged care. It includes notes for providers/workers to help guide the conversation.

Australian Centre for Evidence Based Aged Care - Resources
This resource provides a collection of tools and guidelines for improving person-centred care in aged care settings. It includes assessments on care personalisation, pain management, staff-family relationships, and support for sexuality and decision-making for people with dementia.
This resource was developed by a state/territory government or organisation and therefore its applicability and usefulness may be limited.
First Nations – Workplace poster – Standard 3 Care and services
These workplace standards posters demonstrate the strengthened Standards and what they mean for aged care providers and workers. You can print these out and display them around your workplace.

First Nations - Stakeholder Communications Toolkit
This Toolkit is designed for First Nations stakeholders including providers, workers and others involved in providing aged care services for First Nations people. We’ve developed it to make it easy for you to share relevant resources with your networks and members

Aboriginal and Torres Strait Islander Discussion Starter – Working Out What’s Right For You
This resource includes information and tools to support thinking and talking about wishes and preferences for care at the end of life. This resource has been developed for Aboriginal and/or Torres Strait Islander peoples, their community, and those working with them. The resource also includes information about identifying decision makers and advance care planning.
Guidelines for pharmacists supporting Aboriginal and Torres Strait Islander peoples with medicines management
This resource describes the professional obligations of pharmacists when supporting Aboriginal and Torres Strait Islander peoples with culturally safe and responsive care and medicines management. It includes information about appropriate and effective processes, desired behaviour or minimum standards of good practice and information about duties and responsibilities.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.

National Aged Care Design Principles and Guidelines
This guide provides guidance on different systems and tools that can be used in residential aged care and community settings. It includes topics such as clinical handover and continuity of care (medication management), information technology systems, My Aged Care, quality improvement, and more. This resource complements Part A: Common clinical conditions in aged care and Part B: General approaches to aged care of the RACGP aged care clinical guide (Silver Book).

National Dementia Action Plan
This action plan outlines practical steps to improve the experiences of people living with dementia, their carers, and families in Australia. It aims to guide government policies, improve care services, raise awareness, and integrate support systems over the next 10 years, incorporating feedback from public consultations and stakeholders.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.
Creating safe and inclusive care for Forgotten Australians and Care Leavers
This resource provides guidance for creating safe, inclusive aged care for Forgotten Australians and Care Leavers, focusing on trauma-informed practices. It supports providers in recognising unique needs, avoiding re-traumatisation, and promoting respect and sensitivity in care environments.
National Aboriginal and Torres Strait Islander Flexible Aged Care Program
This resource provides information on the National Aboriginal and Torres Strait Islander Flexible Aged Care Program. The program funds flexible and culturally appropriate aged care services for Aboriginal and Torres Strait Islander communities, mainly in rural and remote areas. It covers service provider requirements, funding processes, and adaptations to ongoing aged care reforms.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.
National Consensus Statement - Essential elements for recognising and responding to acute physical deterioration
This consensus statement outlines essential elements for recognising and responding to acute physiological deterioration in healthcare settings. It covers clinical processes like vital signs monitoring, diagnosis, and rapid response systems, as well as organisational aspects such as leadership, education, and evaluation. It provides generic information that can be applied to the aged care setting.
This resource may refer to information that will be updated from 1 November 2025 to align with the new Aged Care Act and Quality Standards.

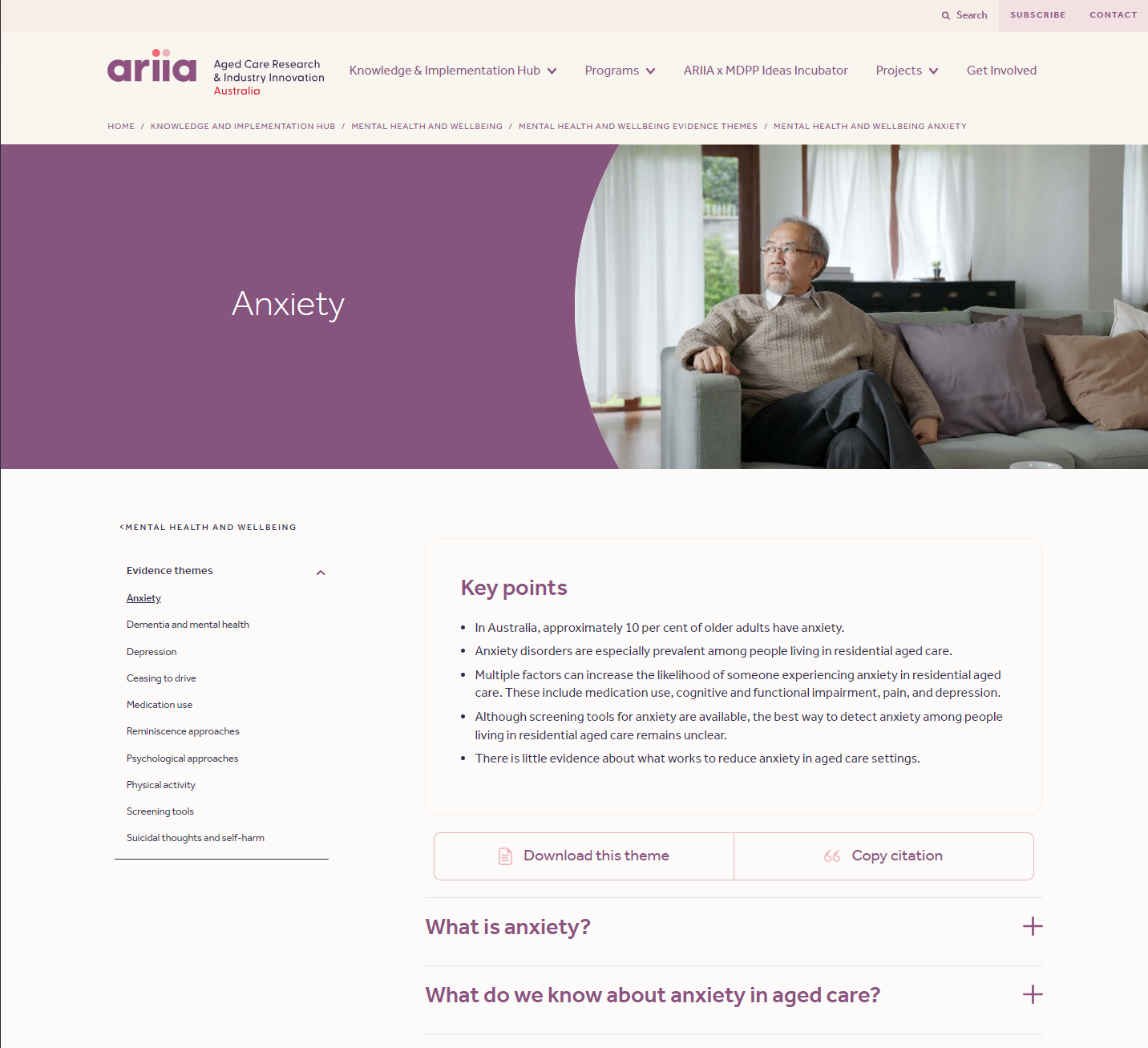
Mental health and wellbeing - Anxiety
This resource provides information on anxiety among older adults, especially those in residential aged care. It outlines risk factors, detection tools, and effectiveness of non-pharmacological interventions such as reminiscence therapy and cognitive behavioural therapy. It also provides guidance on what both individuals and organisations can do to prevent and manage anxiety effectively.